Press release from the University of Birmingham
Peer Reviewed | Experimental | Mice
Research published today shows that an immunopeptide called PEPITEM could provide a revolutionary approach to reducing the risk of obesity-related diseases such as type 2 diabetes and hepatic steatosis (fatty liver).
PEPITEM was first identified in 2015 by University of Birmingham researchers who described its role in the immunomodulatory adiponectin-PEPITEM pathway that is dysregulated in immune-mediated inflammatory diseases, including rheumatoid arthritis and type-1-diabetes.
The latest research, published in Clinical & Experimental Immunology, highlights the potential for PEPITEM as a novel therapy to reduce systemic inflammation and tissue damage that underpins the onset of obesity-related co-morbidities.
The research team was led by Dr Helen McGettrick and from the University of Birmingham’s Institute of Inflammation and Ageing. She said: “Obesity causes low-grade systemic inflammation, that alters the function of cells in the immune system and also stromal cells that are resident within tissues, increasing the risk of developing diseases in organs across the body. Despite this, we know very little about exactly how obesity induced inflammation drives pathology in non-adipose tissues. We’ve shown a completely new therapeutic route, which could provide new drugs to tackle the root cause of the obesity-related conditions by preventing the damage caused by systemic inflammation.”
The researchers used a mouse model of obesity to investigate whether PEPITEM, delivered by a slow-release pump, could prevent or reverse the effects of a high fat diet (HFD) on insulin-producing cells in the pancreas and immune cell migration into various tissues.
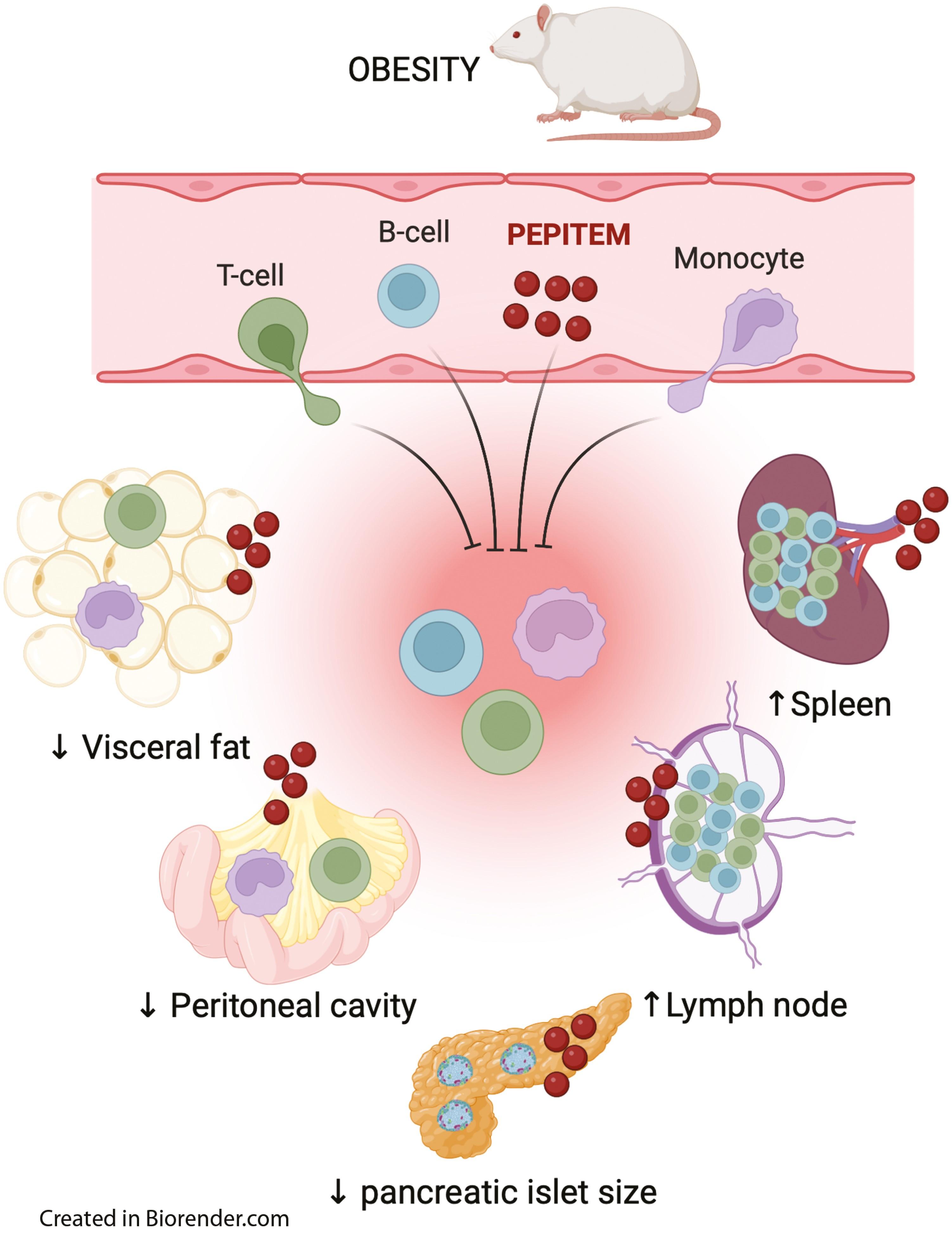
The prophylactic arm of the study investigated the effect of PEPITEM administration over a 6-week period, with mice concurrently fed HFD. The results showed significant reductions in the enlargement of pancreatic islet insulin-producing beta cells (stromal cells), the number of CD4+ T cells in the visceral adipose tissue (VAT) and the peritoneal cavity, and the number of macrophages in the peritoneal cavity compared to controls.
Similar results were shown in the therapeutic arm, where mice were fed HFD for 6 weeks prior to implantation of slow-release pumps for an additional 6 weeks. Here, the group also observed a reduce in the number of T and B-cells in the blood, with a concomitant increase in these cell types seen in secondary lymphoid tissues (spleen, inguinal lymph node). These findings indicate that PEPITEM systematically modulates leukocyte trafficking through tissues, potentially reversing the effects of the obesogenic diet on these body compartments.
Dr Asif Iqbal from Birmingham’s Institute of Cardiovascular Sciences co-led on the project. He commented “The original description of the peptide would have led you to believe that the effects were very much T cell specific, however, the evidence from this study suggest that PEPITEM has much broader effects across multiple leukocyte and stromal populations which will open up multiple lines of exciting new research.”
Professor Ed Rainger from Birmingham’s Institute of Cardiovascular Sciences led the team that first identified PEPITEM. He commented: “We are all very excited about these latest results. PEPITEM is a naturally occurring peptide. We have already shown it has effects on several organs and now for the first time we have shown that PEPITEM is effective in a model of a disease process that is not driven by the immune system.”
Dr McGettrick added: “Obesity is a global health challenge, with numbers of obese adults and children rising at an alarming rate, and many suffering from obesity-related co-morbidities. Collectively these conditions have an enormous impact on global economies, estimated at over 2% of global gross domestic product. Current strategies to reduce obesity focus on modifying lifestyle choices, such as increasing exercise or encouraging weight loss. These can be supplemented with more drastic surgical interventions, and the use of medical drugs to treat obesity-associated co-morbidities. We have now shown that PEPITEM may provide a novel, alternative therapeutic strategy, which may be particularly beneficial in individuals at risk of obesity related diseases.”
University of Birmingham Enterprise had already filed patent applications covering PEPITEM compositions and therapeutic uses, and has now filed a further application covering its use in the use in the prophylaxis or treatment of obesity-associated inflammatory conditions including chronic low-grade systemic inflammation and pancreatic beta-cell damage.
ENDS
PEPITEM modulates leukocyte trafficking to reduce obesity-induced inflammation is published in Clinical & Experimental Immunology, and available at doi.org/10.1093/cei/uxad022.
For further media information please contact Ruth Ashton, University of Birmingham Enterprise, email: r.c.ashton@bham.ac.uk.
For enquiries about licensing or IP please contact Helen Dunster, University of Birmingham Enterprise, email: h.dunster@bham.ac.uk.
About the University of Birmingham
The University of Birmingham is ranked amongst the world’s top 100 institutions, and its work brings people from across the world to Birmingham, including researchers and teachers and more than 6,500 international students from nearly 150 countries.
About Clinical & Experimental Immunology
Clinical & Experimental Immunology is an official journal of the British Society for Immunology, the leading UK membership organisation working with scientists and clinicians from academia and industry to forward immunology research and application around the world. The BSI community consists of more than 4,000 immunologists, creating a powerful voice to advocate for immunological science and health for the benefit of society.
