BiteSized Immunology: Organs & Tissues

Stem cell transplantation
Stem cell transplantation (SCT) is widely used to treat haematological malignancies such as lymphomas, multiple myeloma and myeloid/lymphoblastoid leukaemias. It is potentially applicable as a treatment for some solid organ tumours such as breast cancer and renal cell carcinoma, and is increasingly used to treat non-malignant conditions. The principle is to ablate the immune system and replace it with haematopoietic stem cells from either the patient (autologous-SCT), or from a HLA-matched donor (allogeneic-SCT).
There are different methods for harvesting stem cells. Either cells can be removed directly from the donor’s bone marrow cavity, or the donor can be given granulocyte colony stimulating factor (G-CSF) to mobilise their stem cells to the peripheral blood where they can be harvested. Cord blood can also be used as a source of stem cells. Following the patient’s conditioning, the donor stem cells are infused and migrate to the bone cavities to repopulate the immune system through homeostatic mechanisms. The time of full reconstitution varies between patients and is often dependent on the conditioning regimen.
Myeloablative conditioning ablates the patient immune system using a combination of high-dose radiotherapy and immunosuppressive drugs such as cyclophosphomide or busulphan. This is a highly toxic treatment so the number of patients that could be treated by SCT is limited to those who are fitter and often younger in order to survive the conditioning. Other less intensive conditioning (non-myeloablative or reduced intensity conditioning [RIC]) regimens have been developed more recently, using different chemotherapeutic agents and/or lower doses of radiation which has increased the number of patients for whom SCT is a treatment option.
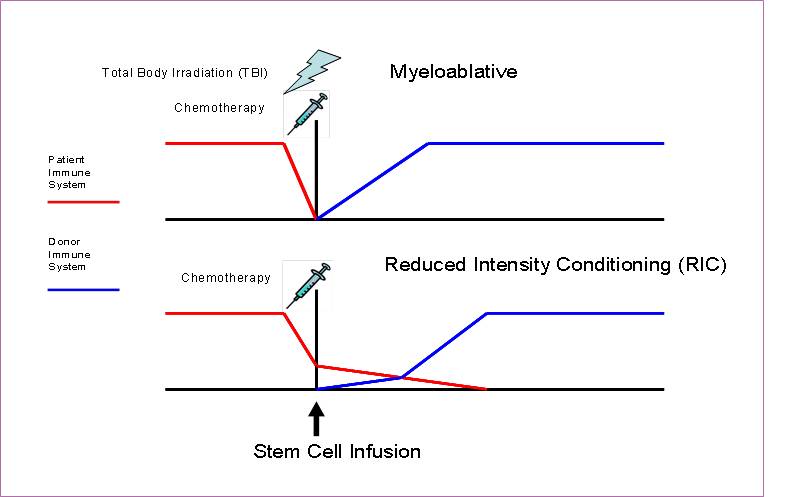
Due to the non-myeloablative nature of the reduced intensity conditioning, following infusion there is a period of mixed-chimerism with both patient and donor cells present. The donor cells should eventually out-compete, leading to the immune system becoming fully donor (Figure 1).
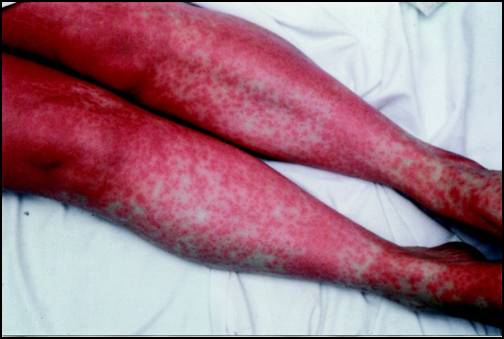
Donors are selected on the basis of HLA-compatibility. The more closely matched the donor and recipient are, the less risk of potentially life-threatening graft-versus-host disease (GvHD) where the new donor immune cells attack recipient tissues, often skin, gut and liver (Figure 2). This can be very debilitating or even fatal.
An important effect following SCT is graft-versus-leukaemia (GvL), which is essential to prevent relapse when treating malignant disease. Both of these effects are thought to be mainly T-cell mediated and GvHD incidence is associated with decreased risk of relapse. Studies have shown that one group of important GvL targets are haematopoietically expressed minor histocompatibility antigens (mHAgs), such as HA-1. However it has also been observed that there are GvL reactions following syngeneic transplantation which are unlikely to be caused by mHAg mis-matches, suggesting that GvL could also have a tumour-specific component. This could potentially be directed against tumour-specific antigens such as the cancer-testis antigen (CTAg) family of tumour proteins, or antigens such as PRAME which can be overexpressed by tumours. Although cancer patients may develop tolerance to tumour-associated antigens, SCT can facilitate development of effective immune responses as the donor system is unlikely to have become tolerised to these cancer proteins.
Occurrence of GvHD presents problems, but has been linked to a decrease in relapse risk, probably due to GvL. Consequently, there is much research interest in trying to enhance the GvL effect whilst simultaneously reducing GvHD.
© The copyright for this work resides with the author.
