BiteSized Immunology: Cells

Eosinophils
Eosinophils are major effector cells in the immune system. They have a beneficial role in host defence against nematodes and other parasitic infections and are active participants in many immune responses. However, eosinophils can also be damaging as part of the inflammatory process of allergic disease.
Eosinophil accumulation and inappropriate activation causes symptoms and pathology in allergic asthma. Eosinophils make up approx 0.5-1% of the white blood cells (leukocytes) in normal individuals, but this proportion is often raised to 3-5% in people with allergic symptoms, and can be much higher in those exposed to parasitic worms.
Human eosinophils are approximately 8μm in diameter and are identified by their bi-lobed nucleus, pink staining with eosin and characteristic cytoplasmic granules. Differentiation of haemato-poietic progenitors to eosinophils in the bone marrow is governed by SCF, IL-3, IL-4, GM-CSF and CCL11. IL-5 and CCL11 then act in concert to drive final differentiation, maturation and release of eosinophils from the bone marrow into the bloodstream.
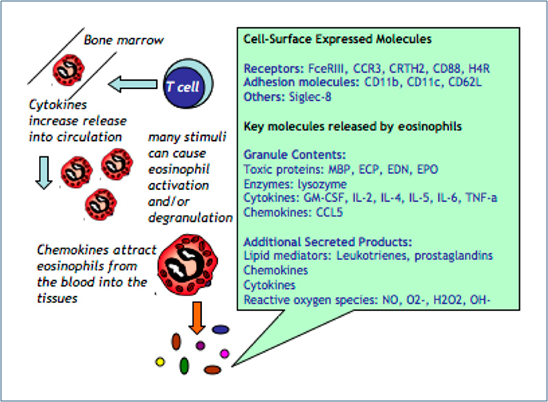
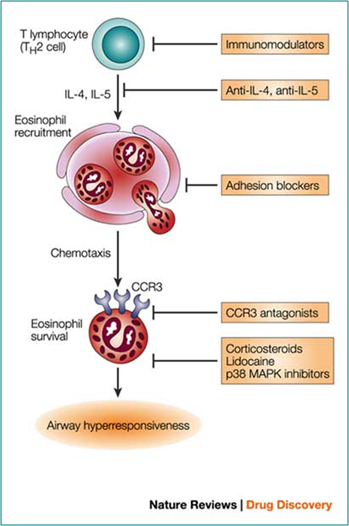
Eosinophils express a range of receptors, e.g. CCR3, the receptor for CCL11, which allow them to respond to a multitude of cytokines, chemokines and lipid mediators. Eosinophils are recruited from the blood into the tissues at sites of inflammation. Upon activation eosinophils can release an array of inflammatory mediators (Figure 1). Cytotoxic proteins MBP, ECP, EDN and EPO are unique to eosinophils and are important in the defense against extracellular parasitic infections but may also cause excessive tissue damage in allergic conditions. There are many strategies to limit eosinophil-related tissue damage (Figure 2).
© The copyright for this work resides with the author.
