BiteSized Immunology: Cells

Th17 cells
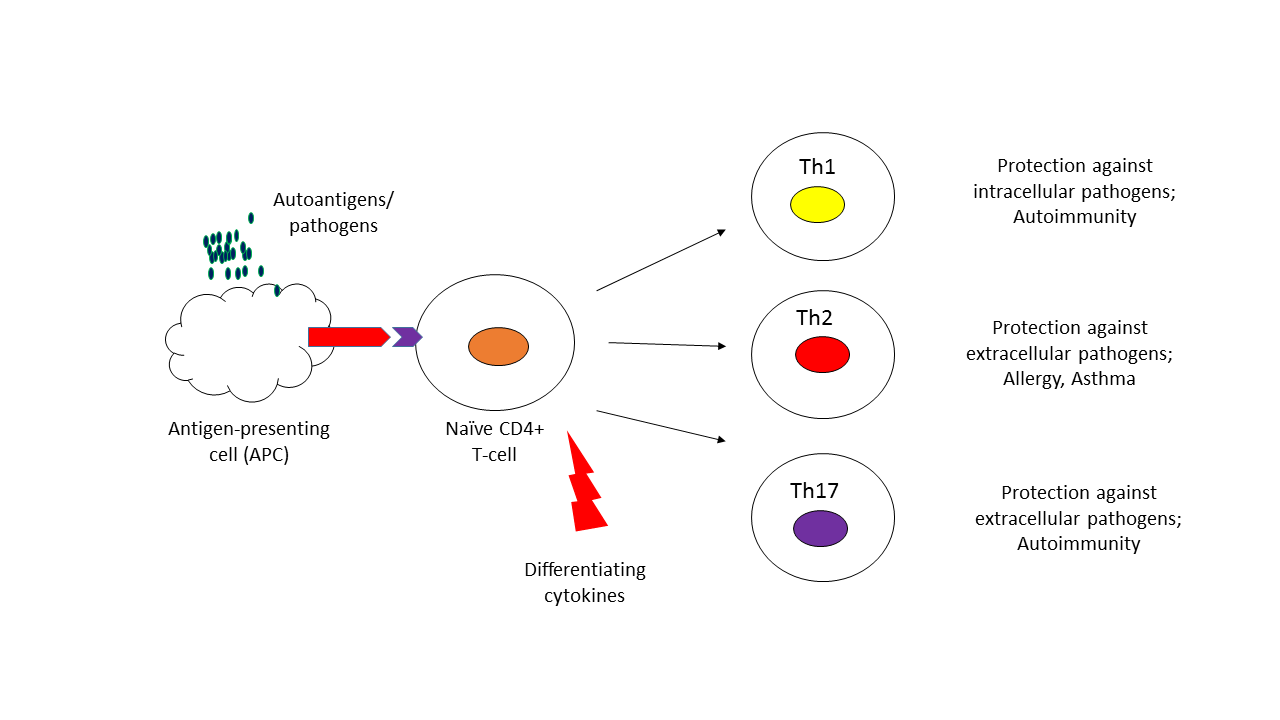
CD4 T cells play a key role in the functioning of a healthy immune system. They assist B cells to make antibodies, activate the microbe killing capacity of macrophages and recruit other immune cells to infected or inflamed areas of the body. These activities are orchestrated through their production of various cytokines and chemokines. It has been known for some time that uncommitted CD4+ T-cells can differentiate into Th1 or Th2 cells, based on the prevailing pro-inflammatory/anti-inflammatory environment, and that these activated Th1 and Th2 cells had distinct cytokine production patterns and functions.
Generally, Th1 cells were associated with the eradication of intracellular pathogens whereas Th2 cells were heavily involved in responses against extracellular pathogens and parasites. Uncontrolled Th1 responses were implicated in autoimmunity and aberrant Th2 responses were associated with allergy and asthma development. However, this model did not explain the observation that a deficiency in Th1 signalling and/or cytokines still allowed the development of autoimmune diseases such as rheumatoid arthritis and multiple sclerosis. More recently (2006) a third subset of CD4 T cells, Th17 cells, which have a pro-inflammatory bias was identified. Subsequent research using animal models and human studies has demonstrated a key role for Th17 cells in the immune system’s defence against extracellular bacteria and fungi as well as the development of autoimmune diseases, mediated by the secretion of IL-17 by these cells. The secretion of IL-23 from antigen-presenting cells such as dendritic cells, which have been activated by the uptake and processing of pathogens, in turn activates Th17 cells.
© The copyright for this work resides with the author
