BiteSized Immunology: Pathogens & Disease

Pathogenic Yersiniae
Pathogenic bacteria of the Yersinia genus cause three types of disease, namely: plague (Yersinia pestis; Figure 1), pseudotuberculosis (Yersinia pseudotuberculosis) and yersiniosis (Yersinia enterocolitica). In achieving this, these pathogens exhibit common ways of manipulating the mammalian host‘s immune system to achieve their own survival (see related articles).
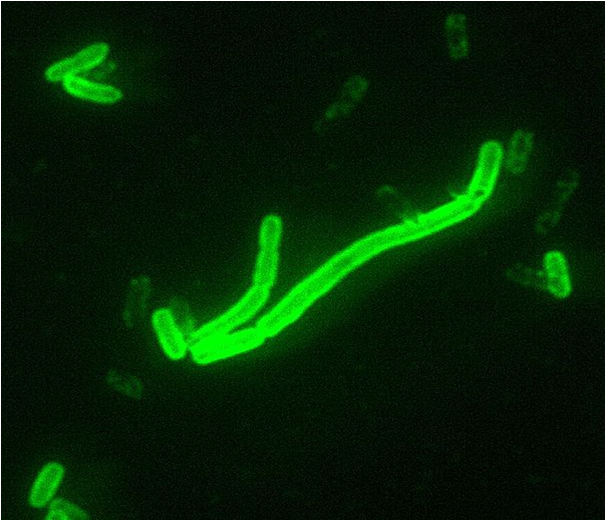
Plague
The etiological agent of plague is Yersinia pestis. Although an ancient disease, which has caused many millions of deaths in history, plague is still endemic in parts of the world today and thus is still of concern. Infection with Y.pestis causes approximately 3000 deaths per annum globally (World Health Organization figures) and whilst infection rates in Asia have remained steady, the incidence of plague has been increasing in Africa. Yersinia pestis is a small oval, Gram-negative, capsulate coccobacillus with a characteristic bipolar staining phenotype (occurring at either end of the bacillus). Y.pestis is thought to have evolved over thousands of years from the ancestral species Y.pseudotuberculosis, to become a flea-vectored pathogen and in the process has acquired plasmid DNA encoding for virulence factors which endow it with anti-phagocytic and anti-host cell activity, and which allow it to evade host immune defences. For example, Y.pestis produces tetra-acylated (rather than hexa-acylated) lipopolysaccharide thus evading TLR4 activation in the host; and Y.pestis is recognised only weakly by TLR2 receptors, thus avoiding macrophage activation. Y.pestis has also inactivated its O-antigen genes, allowing the plasminogen activator (PLA) protease to be fully functional at the bacterial surface. PLA degrades host plasminogen, promoting the dissemination of bacteria from the site of infection to tissues and organs. Additionally, Y.pestis produces a fibrillar adhesin (pH6 antigen) which binds host apo-B lipoprotein to the bacterial surface, thus protecting the bacteria from phagocytosis; and Y.pestis also resists the effects of complement, through expression of the outer membrane adhesion protein (the ail adhesin) and other genome-encoded virulence factors.
As with some other Gram-negative bacterial pathogens, on close contact with a host cell in vivo, Y.pestis produces a hollow needle-like projection through which effector proteins (Yersinia outer proteins, Yops) are translocated directly into the host cell. This is the so-called type three secretion system. These effectors are variously cytotoxic, anti-phagocytic, or anti-inflammatory and generally promote the apoptosis of host cells and thus the survival of bacteria in the host. By all these means, Y.pestis counters innate immune defences and achieves dissemination in the host to establish a potentially fatal bacteremia.
Reservoirs of Y.pestis are maintained in wild rodent species, and plague is most commonly transmitted to man by the bite of an infected flea. Where this is the route of transmission, the syndrome which develops in the man is bubonic plague which entails the development of grossly-enlarged lymph nodes (the bubos )draining the site of infection and which has the potential to develop into a generalised systemic infection (septicaemic plague) or to form a secondary infection in the lung (pneumonic plague). The latter infection then has the potential to be transmissible as an aerosol to naïve individuals to establish a primary pneumonic plague infection.
Antibiotics such as the fluoroquinolones can be used for the therapy of plague, but the likely success rate is inversely proportional to the time elapsed post-infection before therapy is started. A number of killed whole-cell vaccines have been approved for the prophylaxis of plague in those who may be exposed to the bacterium through travel to endemic areas, or as an occupational hazard. Although thought to be efficacious against bubonic plague, these may not protect against pneumonic plague. A next generation recombinant sub-unit vaccine (rF1V) is in advanced clinical trials and when approved is expected to be more comprehensively efficacious, particularly in preventing the development of pneumonic plague.
© The copyright for this work resides with the author.
